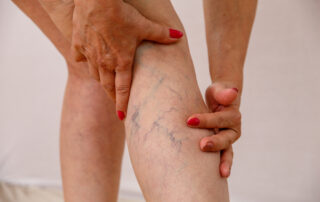
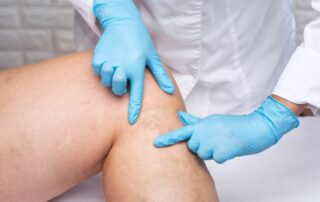
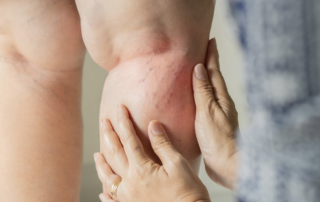
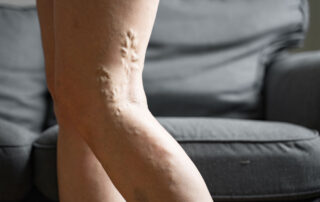
Varicose Veins vs. Spider Veins: What’s The Difference and When Should You See A Specialist?
Medically reviewed by Dr. Billy Kim, MD, FACS • The Vein Centre Have you noticed visible veins on your legs and wondered if they are normal or cause for [...]