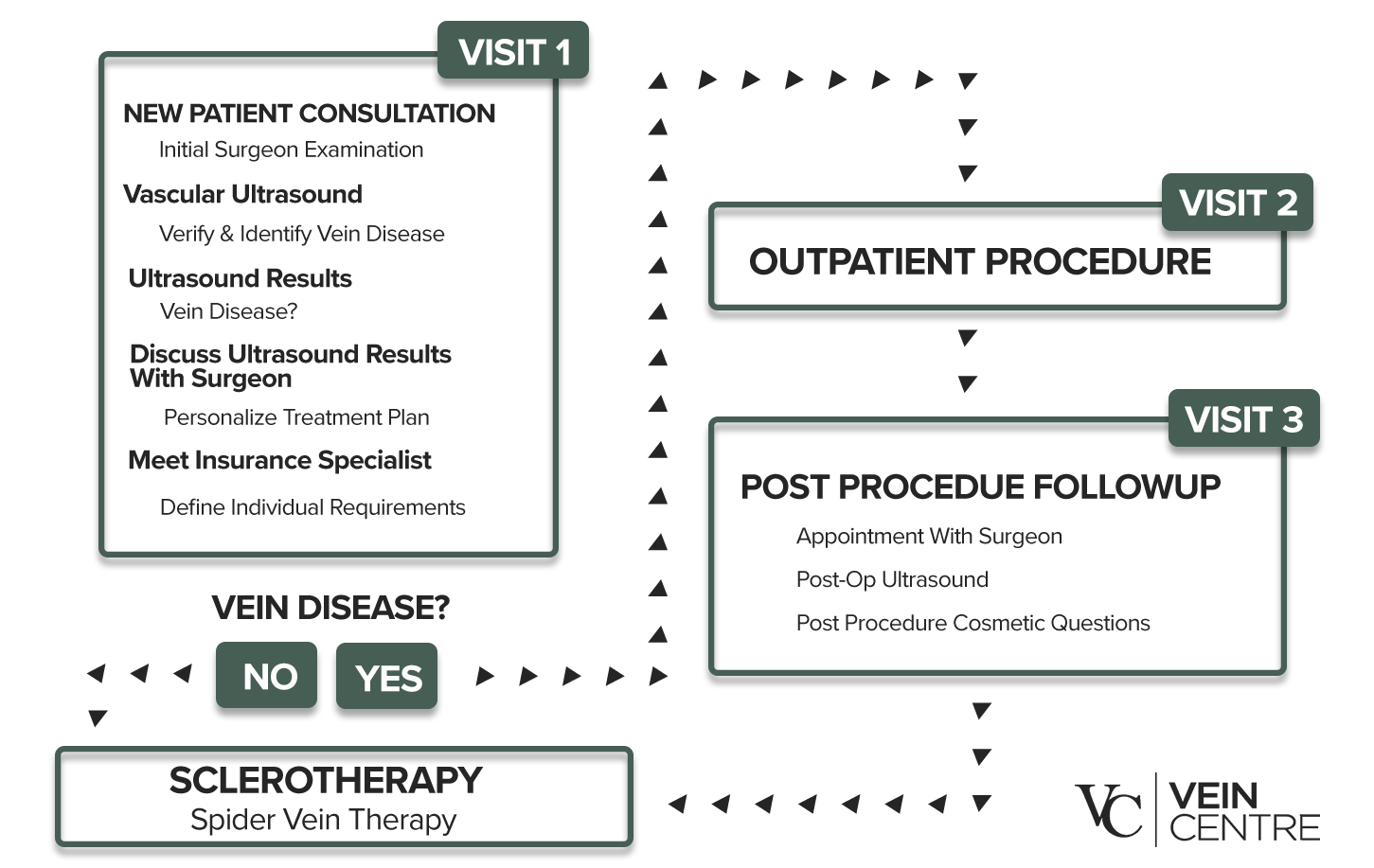
VEIN SOLUTIONS BLUEPRINT. Vein Treatments Are as EASY as 1-2-3
VEIN TREATMENT IN BELLE MEADE, FRANKLIN, AND MT. JULIET
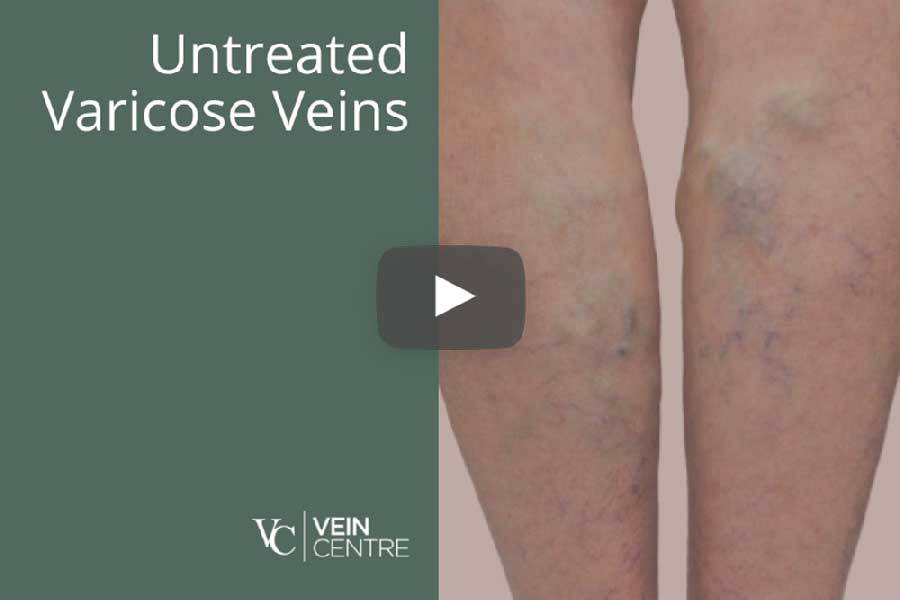
Whether you’re suffering from varicose veins or spider veins and live in Williamson County in Middle Tennessee, the professionals at the Vein Centre are here to help. Learn about the different vein treatments we provide for vein disease. Then give us a call and schedule a consultation so we can find the best treatment for you.
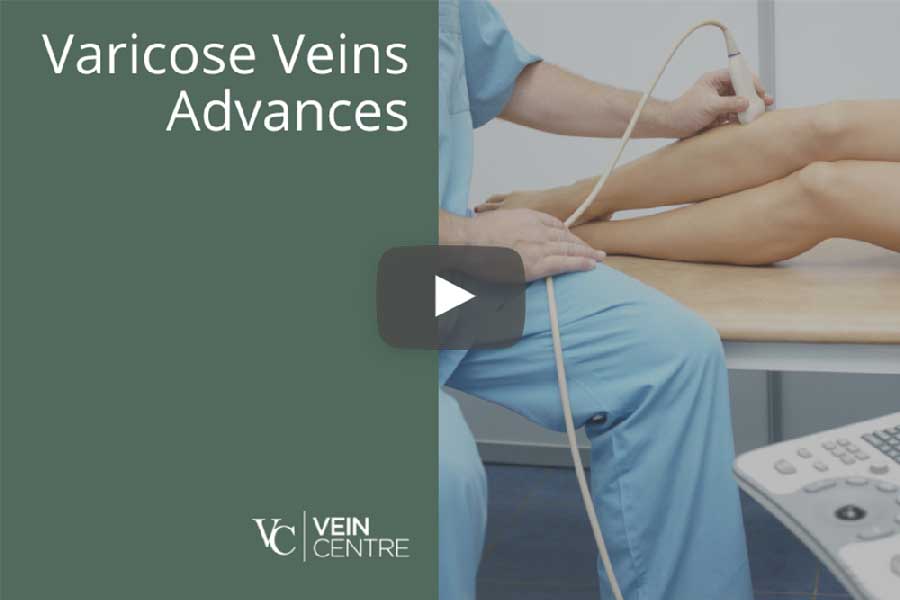
Vein surgery using radiofrequency ablation: after local numbing, a laser fiber is inserted into a straight vein, usually the saphenous vein. Heat energy at the laser tip welds the vein walls together as the laser is pulled down through the vein. This closes the vein and stops the downward flow of blood (reflux) that is responsible for the varicose veins and aching congestion in the leg.
The in-office, laser ablation procedure takes approximately 45 minutes, and the patient may immediately resume normal activities. A tape strip closes the skin site and compression stockings are required to be worn following the procedure. This procedure has proven high long-term success rates, low complication rates, and rapid recovery.
The radiofrequency procedure can be performed under local anesthesia in the physician’s office. Patients have reported little, if any, pain during the procedure, and most return to normal activity within a day. Some common side effects include temporary tenderness and numbness. You can expect a noticeable improvement within 1 to 2 weeks, with good cosmetic outcomes and little to no scarring. How successful is laser ablation?
Results have been extremely favorable and success rates are equal to those associated with the surgical ligation and stripping of veins. Most patients require no additional treatment. However, a small percentage of patients may require additional therapy such as sclerotherapy. What are the side effects?
As with any medical procedure, side effects may occur with vein treatments. However, minimal side effects have been documented with this procedure. Bruising and minor soreness can be expected and can be treated with over-the-counter pain relievers. A small percentage of patients have experienced temporary numbness in the treated area of the leg.
A new treatment for closing straight veins (usually the saphenous vein).
The VenaSeal™ closure system is the only non-tumescent, non-thermal, non-sclerosant procedure that uses a proprietary medical adhesive delivered endovenously to close the vein. The adhesive is injected into the vein after local numbing, causing the walls to heal together, stopping the reflux.
This unique approach eliminates the risk of thermal nerve injury when treating the small saphenous vein. The procedure is administered without the use of tumescent anesthesia, avoiding patient discomfort associated with multiple needle sticks. Another advantage over other vein treatments are less numbing required and no need for stockings after the procedure.
Varithena® improves symptoms related to or caused by varicose veins, and the appearance of varicose veins. Varithena® improves vein appearance and 5 key varicose vein symptoms:
• Heaviness
• Achiness
• Swelling
• Throbbing
• Itching
A manufactured foam combining sclerosant with medical carbon dioxide and oxygen is injected into straight vein segments (usually the saphenous vein) or into varicose veins. Varithena requires less numbing than the laser closure procedure though long-term success rates at closing the vein appear to be slightly better with the laser treatment. Varithena procedure is FDA approved and was given insurance coverage by most major health insurers January 2018.
SCLEROTHERAPY FOR SPIDER VEINS
Sclerotherapy involves a series of injections of a sclerosing medicine into the tiny veins. For slightly larger spider veins, medical carbon dioxide can be added to the liquid sclerosant to make a foam that is injected in the same manner.
This procedure takes approximately 30 minutes, depending on the size of the veins, and requires only the wearing of support hose or stockings for several days following the treatment to optimize its effects. For the best results, sclerotherapy treatments are usually scheduled four to six weeks apart.
Most patients have satisfactory results following their treatment plan. Some patients may notice that their legs look worse before they look better. This is common. Clearing of the veins after sclerotherapy is gradual and usually, additional treatments are necessary based on the number of veins and their size. Positive results are usually visible within 4 weeks following the first treatment.
What are the side effects? As with any procedure, there is always the possibility of side effects. Some of the most common side effects include: Tenderness – the veins may be tender to the touch after treatment and an uncomfortable sensation may run along the course of the vein. This discomfort is usually temporary. Some patients complain of an itchy sensation after treatment. Firmness in the treated area can occur and is minimized by the use of support hose.
Trapped blood may cause a discoloration, although this may leave hyperpigmentation up to one year. Transient Hyperpigmentation – Approximately 20% of patients who undergo sclerotherapy notice discoloration after treatment. This usually fades in several months. There is a 1% chance of hyperpigmentation continuing after one year. Patients frequently notice a brown discoloration, which fades in a couple of months – at most within a year.
Ambulatory phlebectomy is an outpatient procedure usually performed under local anesthesia and the patient can usually return to normal routines immediately. After local numbing, tiny incisions are made over clusters of bulging varicose veins and a hook is used to disrupt and remove the veins in pieces.
No stitches are required, and the incisions look like freckles in eight weeks. A compression stocking is worn for a week after the procedure but may be removed to bathe. This minimizes swelling and discomfort and allows for proper healing. Side effects are rare but include paresthesia, bruising and hematoma.
A blood clot in the deep veins of the leg can break free, going through the heart to lodge in the lungs (pulmonary embolism), which can be life threatening. Early treatment with blood thinners greatly reduces that risk.
With the passage of weeks and months, the clot sticks to the vein wall and is less likely to break free. The clot is then partially or completely reabsorbed, allowing the blood to drain more freely out of the leg and back up to the heart. However, in up to half of cases, the clot is not completely reabsorbed and turns into scar tissue that prevents the leg veins from draining properly. This is called the post-phlebitic syndrome and over many years can lead to leg swelling, skin thickening, skin darkening (hyperpigmentation) and even skin breakdown to chronic venous wounds (ulcers) that can take months to heal and cause lifelong problems.
Traditional treatment has been long term compression stockings to prevent swelling and slow down skin changes. After ulcers form, aggressive treatments, including compression wraps, dressings and even skin grafts are required for weeks to months. Even after the ulcers heal, stockings must be worn permanently to prevent the ulcers from reoccurring. Venous ulcers are common, making up 30% of all patients who have to be treated at a wound center.
Past attempts to surgically remove scar tissue from veins to open up the blood flow have had poor success and were very invasive. In the last several years, much research and progress has been made with new, endovascular (balloon and stent) treatments to open up blocked veins. If the vein can be opened to allow better blood flow, the swelling and progression of skin changes can be improved, lessening the risk of ulcers and problems in the future.
VEIN TREATMENT PATIENT TESTIMONIALS
The Vein Centre’s minimally invasive procedures and laser vein treatments for Nashville and Mt. Juliet residents have been very successful. Read their testimonials to discover how you can feel confident in choosing us for your vein care.