If you have varicose veins, you may not enjoy the look of them. Although unsightly, they are generally not harmful or something to worry about.
Some people choose to have them removed for aesthetic purposes only. For others, though, varicose veins may be a warning sign of other deeper vein health issues. Learn about varicose veins, and when they pose a danger to your health.
What Are Varicose Veins?
The word varicose simply means swollen or unusually dilated. Veins that are varicose are visible, swollen veins that are often blue or purple.
Varicose veins are veins that have been damaged or have become weak. When blood moves through the body, veins carry blood only one way through each vein or blood vessel.
If the valves that control the flow of blood stop working correctly, blood can pool in the vein. This additional pressure and backflow can make the veins fill up, bulge, and start to twist, a lot like how a fast-flowing river appears. When these veins are closer to the skin’s surface, they are visible. So, the main cause of varicose veins is weak veins close to the skin’s surface.
While varicose veins may start as a cosmetic concern, they often progress over time. In early stages, they may only cause mild discomfort. However, without treatment, they can worsen and lead to swelling, skin changes, or even venous disease. Doctors sometimes classify varicose veins by severity to monitor progression and guide treatment.
ARE SPIDER VEINS THE SAME AS VARICOSE VEINS?
Spider veins, or telangiectasias, are small veins visible on the skin’s surface. They are often red, blue, or purple and can appear to “web” out. These veins are harmless and aren’t considered varicose veins. Their existence may be a symptom of poor circulation, which could indicate a higher risk of developing varicose veins.
Since not all spider veins turn into varicose veins, they are considered a cosmetic procedure to have removed. However, often spider veins can progress into becoming varicose veins, so most patients choose to have procedures to remove spider veins in order to prevent varicose veins.
If you notice spider veins, practicing good vein health habits such as regular exercise, elevating your legs, and avoiding prolonged sitting or standing can help reduce your risk of developing larger varicose veins in the future.
When to See a Vein Doctor
While some varicose veins can be normal and don’t pose a health risk, it is crucial to know if they are a health concern. Not treating these veins can result in much more severe conditions.
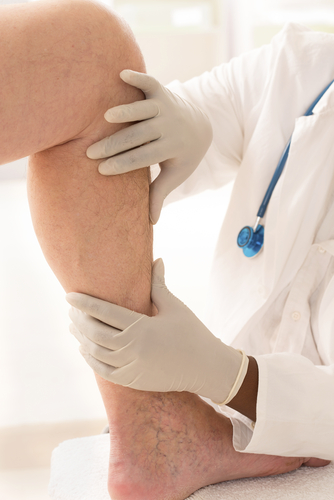
If you are experiencing any of these symptoms, make sure you give your doctor a call and schedule a vein screening. Some vein clinics like the Vein Centre offer online consultations as well. The earlier you can catch a circulatory problem, the better chance you have at correcting it or controlling it.
Common symptoms of varicose veins and spider veins
- Severe and continuous leg pain
- Swelling in the legs, ankles, and feet
- Heaviness or a dull ache in the legs that happens often
- Varicose veins are red and painful or feel warm
- Spontaneous bleeding from veins or bleeding from a slight injury
- Itchy and inflamed skin around veins
- Ulcer and open skin wounds that developed on their own/li>
When to Seek Care Right Away
Most of the symptoms above mean you should schedule a vein screening, but some signs require more urgent attention. Call a doctor immediately if you notice:
- Sudden, severe swelling in one leg
- Intense pain or redness with warmth (possible blood clot)
- Heavy bleeding that does not stop with pressure
If these symptoms occur, do not wait because they could be a sign of deep vein thrombosis (DVT) or another serious vascular issue.
How Serious are Varicose Veins?
While varicose veins may never become a health concern, they have the potential to develop into a vein ailment or disease over many years. These more complex health issues can take years to form, so if you have varicose veins, you should schedule consistent screenings.
When should I worry about varicose veins?
Varicose veins are often a sign of deeper vein issues that could develop into serious or even life-threatening conditions. See a doctor if you experience a sudden increase in swelling or leg pain; these symptoms may indicate a serious problem.
Furthermore, if you leave serious varicose veins untreated for a long time, they can lead to life-threatening conditions.
Leaving unhealthy veins untreated can result in:
- Severe pain: This can feel like a deep ache or heaviness in the limbs.
- Muscle cramps: Cramping can occur when blood pools in the veins instead of flowing through muscle tissue as it should. Leg cramps can happen, especially at night.
- Itching and burning: Leaky blood vessels can cause itching. When little oxygen is able to reach the skin, veins can become itchy and red.
- Blood clots: Also known as phlebitis. Blood clotting can occur as veins become twisted, and the blood flow is not quick enough. Slow-moving blood won’t break up, forming clots as it is stagnant.
- Deep vein clot (thrombus): Also known as DVT or deep vein thrombosis, affects over 200,000 people per year. Leg pain from DVT can worsen as you bend your foot.
- Skin ulcers: A varicose ulcer can occur when blood doesn’t circulate back to the heart effectively. As blood backs up in the veins, pressure builds under the skin, and an open wound may form. Leg ulcers are the most common.
- Pulmonary embolism: PE is a serious condition that occurs when the lung artery is blocked. The blockage occurs when a blood clot makes its way through the bloodstream to the lung. PE causes permanent lung damage.
- Lymphedema: When varicose veins begin to damage the lymphatic system, lymphedema can occur. This condition causes swelling, most often in the feet and toes.
- Cellulitis: If lymphedema has occurred, cellulitis may follow. Cellulitis is a serious skin infection of the soft tissue skin.
- Venous stasis dermatitis: Another skin ailment from unhealthy veins where the skin can become leathery and reddish-brown. In some cases, clear or yellow fluid comes through the skin.
- Dermatitis: Dermatitis is an inflamed, itchy rash from varicose veins. Found on the leg or ankle often.
- Peripheral artery disease: Called PAD for short. When PAD is occurring, the veins aren’t able to provide enough blood flow to the limbs. This condition is likely widespread through the body and can affect the heart and brain, as well.
Steps to Take
While some of these complications are only uncomfortable, others can be life-threatening. If you have any concerns about your circulatory health, it is critical to visit a board-certified vascular surgeon to have a vein health screening. There are several noninvasive tests they can perform to assess the health of your veins.
How do you fix varicose veins? Dr. Roger Bonau, board-certified vascular surgeon at the Vein Centre explains treating varicose veins in this video.
Fortunately, there are treatments for varicose veins. If the pain is mild, there are treatments your doctor can teach you to do self-care at home, such as wearing compression stockings, elevating your feet, increasing exercise, and the use of pain medication. But sometimes a vein requires treatment.
Mild discomfort like itchy varicose veins can be treated with medicated creams, antihistamines, antibiotics, and dressings.
In rare cases, varicose veins can cause skin ulcers and other serious complications. If you have varicose veins, see a doctor right away for treatment options. Many varicose vein treatment options are covered by insurance, and there are several advanced forms of treatment. However, once your veins start to become varicose, there’s often little that can be done to prevent new varicose veins from developing in the future.
During a vein screening, your provider may use an ultrasound to check for clots and measure how well blood is flowing through your veins. Many insurance plans require documentation of these diagnostic tests and a trial of conservative treatments (like compression therapy) before covering advanced procedures.
Vein Health Tips
Vein health can be part hereditary and part lifestyle. Some risk factors like aging, obesity, pregnancy, smoking, and occupations that require sitting or standing can make matters worse.
Try practicing these tips to give your veins a break:
- Don’t sit or stand for long periods.
- If you are sitting for long periods, get up every 30 minutes, and move around.
- Elevate the legs above the heart whenever possible. You can use pillows or the arm of a chair to support your legs.
- Regular exercise can get your blood flowing and relieve veins with pooling blood.
- If you are overweight, eat a healthy diet and try to lose weight.
- Wear compression stockings, especially on long trips or when sitting for long periods of time.
Along with these habits, choosing a fiber-rich diet can ease pressure on your veins by preventing constipation. Reducing salt helps minimize swelling, while staying hydrated and maintaining a healthy weight support overall vein health.
See a Vein Specialist at The Vein Centre in Nashville
The board-certified vascular surgeons at The Vein Centre are trained and experienced in identifying vascular diseases. The Vein Centre’s main goal is to get to the root of the problem for each patient, not just treating the surface veins. Oftentimes, what’s happening on the surface is a result of deeper issues. It’s best to see a board-certified vascular surgeon to know without a doubt how to best treat each specific vein issue.
It is recommended, especially with age or other risk factors, to get regular screenings starting after 30 years of age. If you experience any of the symptoms and discomforts listed above, or are at risk for vein disease, please don’t hesitate to give us a call. The Vein Centre offers many types of vein treatments for venous disease.
Our offices are located near Belle Meade and Mt. Juliet. Visit us in Nashville or Mt. Juliet, Tennessee. To schedule, please call us at 615.269.9007. We would be happy to answer any questions you may have about our vein services.





